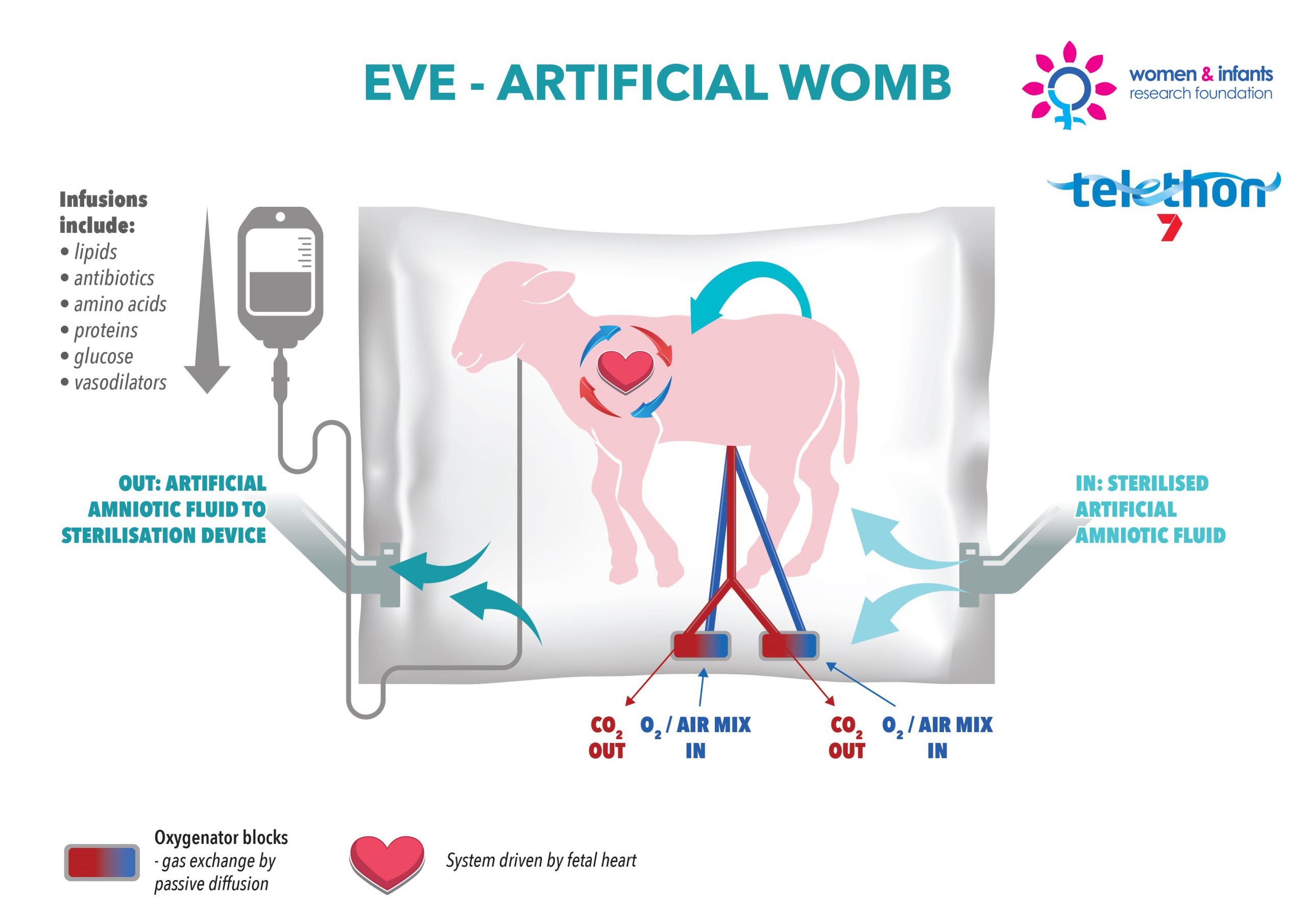
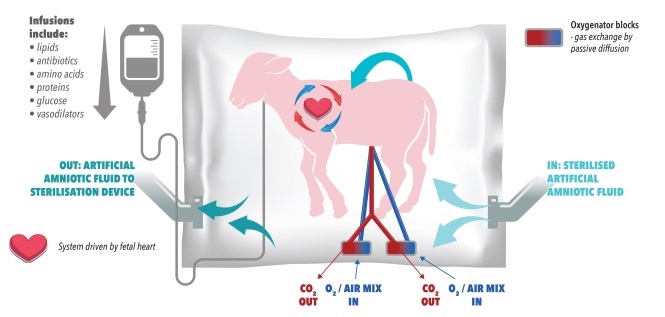
A Western Australian-based research program which proposes an artificial womb as a pioneering medical intervention to save extremely premature babies, has done what few other projects ever have; achieving a perfect score by the key driver of health and medical research in Australia.
The Project Grant, ‘EVE Therapy: A New Life Support System for Preterm Babies Born at the Border of Viability’ was scored as a Category 7 following assessment by the National Health and Medical Research Council’s (NHMRC) Grant Review Panels, placing it in the top 0.1 per cent of all national projects.
The long-standing collaborative program, involving researchers from the Women and Infants Research Foundation, The University of Western Australia and Tohoku University Hospital, Japan, offers new hope for babies born at the border of viability, around 22 to 23 weeks.
Researchers involved in the project have been able to keep preterm lambs alive and well with the EVE Therapy which uses an amniotic fluid bath linked to an artificial placenta.
Crucially, they treat the premature lambs as foetuses rather than small infants, by replicating a womb environment. The lambs continue to grow during the two week-long incubation, and show no ill-effects when they are later delivered.
Head of WIRF’s Perinatal Research Laboratories and Local Chief Investigator, Associate Professor Matt Kemp, said the NHMRC result was great reward for the entire project team and represents a significant milestone in the technology’s future implementation into clinical use.
“If we are to improve outcomes for babies born at the border of viability we must recognise that they are not ‘small babies’; rather, they are a unique patient demographic that, due to their extremely underdeveloped lungs and limited cardiovascular capacity, require an entirely different treatment approach from older preterm infants.
“This project is a wonderful example of international collaboration; it brings together leading academic researchers from Japan and Western Australia, and is undertaken in close partnership with one of Japan’s foremost biomedical technology companies, Nipro Corporation” he said.
Associate Prof Kemp said the potential significance of the project was enormous.
“Nothing we have now is able to extend survival beyond 22 – 23 weeks gestation and usually with great costs to the child’s future physical and mental health. What today might be considered as futuristic technology might soon not be so futuristic and might be standard of care.”
WIRF Chief Scientific Director, Professor John Newnham said Assoc Prof Kemp was a true pioneer of the new era of perinatology.
“He is one of only a handful of applicants applying to the NHMRC Project grant process to achieve a perfect score of seven for any submitted project application history, said Prof Newnham.
“He has ensured that Western Australia is a global leader in research into perinatology and finding new solutions to the problems that emerge during the perinatal period. His research spans new technologies but he embeds his research in an environment to support clinical translation.
“Not only do we have some of the best minds in the field working on this much needed treatment, we also have a clear pathway for moving the results of our work beyond the laboratory and into clinical use.”
Perth-based researchers, including visiting Fellow Dr Haruo Usuda, work year-round with researchers from Tohoku University Hospital in Sendai (led by A/Prof Masatoshi Saito and Dr Shimpei Watanabe) and the Artificial Placenta Development Team at Nipro Corporation in Osaka (led by Mr Shinichi Kawamura).
The NHMRC outcome is the latest in a long list of achievements for the research project which includes its recognition as one of the Top 10 Science Stories of 2017 by the Australian Science Media Centre, and most recently, being featured at the 2018 Ars Electronica Festival in Linz, Austria.
This work has been supported by significant seed funding provided by the Western Australian Department of Health.