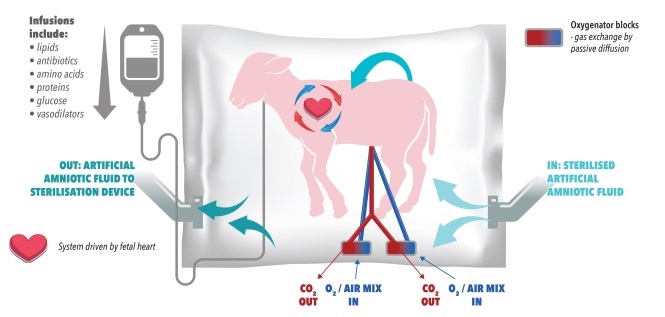
A major advancement in pioneering technology based around the use of an artificial womb to save extremely premature babies is being hailed as a medical and biotechnological breakthrough.
Recently published in the leading medical publication, The American Journal of Obstetrics & Gynecology, the study presents world-first data demonstrating the ability of an artificial placenta-based life support platform to maintain extremely preterm lamb fetuses (600-700g); equivalent to a human fetus at 24 weeks of gestation.
Head of WIRF’s Perinatal Research Laboratories and Local Chief Investigator, Associate Professor Matt Kemp, said that whilst previous research had demonstrated the feasibility of extended survival with artificial placenta technology in late preterm fetuses, there was no published evidence that demonstrated the use of the platform to support extremely preterm fetuses – the eventual clinical target of this technology.
“For several decades there has been little improvement in outcomes of extremely preterm infants born at the border of viability (21-24 weeks gestation),” Assoc Prof Kemp said.
“In the AJOG study, we have proven the use of this technology to support, for the first time, extremely preterm lambs equivalent to 24 weeks of human gestation in a stable, growth-normal state for five days.
“This result underscores the potential clinical application of this technology for extremely preterm infants born at the border of viability. In the world of artificial placenta technology, we have effectively broken the 4 minute mile.”
Assoc Professor Matt Kemp said the latest findings represent a significant milestone in the technology’s future implementation into clinical use.
“If we are to improve outcomes for babies born at the border of viability we must recognise that they are not ‘small babies’; rather, they are a unique patient demographic that, due to their extremely underdeveloped lungs and limited cardiovascular capacity, require an entirely different treatment approach from older preterm infants.
“The technology was designed to revolutionise the treatment of severely premature newborns. The goal is to offer a bridge between a natural womb and the outside world to give babies born at the earliest gestational ages more time for their fragile lungs to mature.
“With additional refinement, what today might be considered as futuristic technology might soon not be so futuristic and might be standard of care.”
The EVE Therapy project brings together leading academic researchers from the Women and Infants Research Foundation, The University of Western Australia and Tohoku University Hospital, Japan, and is undertaken in close partnership with one of Japan’s foremost biomedical technology companies, Nipro Corporation.
Perth-based researchers, including Visiting Fellow and project development head Dr Haruo Usuda, work year-round with researchers from Tohoku University Hospital in Sendai (led by A/Prof Masatoshi Saito and Dr Shimpei Watanabe) and the Artificial Placenta Development Team at Nipro Corporation in Osaka (led by Mr Shinichi Kawamura).
The AJOG paper is the latest in a long list of achievements for the research project which includes:
Achieving a perfect score by the key driver of health and medical research in Australia (NHMRC) placing it in the top 0.1 per cent of all national projects,
Recognised as one of the Top 10 Science Stories of 2017 by the Australian Science Media Centre,
Featured at the 2018 Ars Electronica Festival in Linz, Austria.
This work has been supported by the Channel 7 Telethon Trust, the Department of Health, Government of Western Australia, Nipro Corporation, the Women and Infants Research Foundation and the National Health and Medical Research Council.
The paper, ‘Successful treatment of extremely preterm ovine fetuses with ex-vivo uterine environment therapy’ has been published online at The American Journal of Obstetrics & Gynecology and can be viewed here.